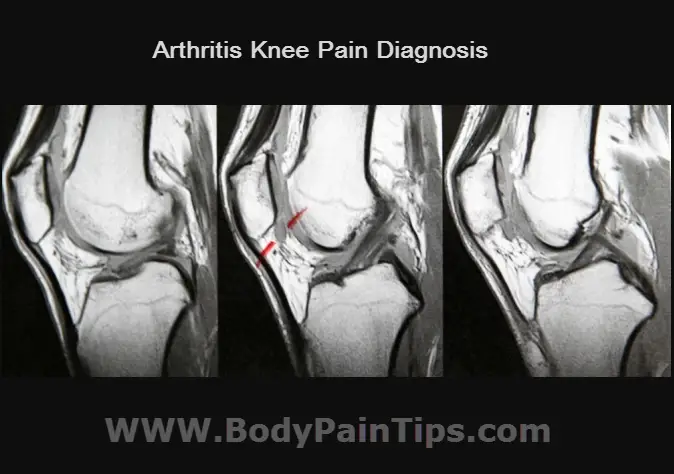
How To Diagnose Arthritis Knee Pain
Your doctor will likely ask when you noticed your knee pain, how it feels and whether you’ve had any previous injuries. He or she also may ask about your physical and athletic habits and goals, which may help determine the best treatment for your situation. Your doctor may begin with a physical examination that includes feeling around the painful area and testing ligament and tendon strength.
Other tests that are helpful include: the X – ray, these may be taken from several angles, usually provide a good way to diagnose arthritis and are particularly useful for assessing joint space narrowing that indicates early wear of the cartilage; the Magnetic Resonance Imaging (MRI), this type of scan can help your doctor visualize the inside of your joints and bones. Although this is not all that helpful in diagnosing osteoarthritis, it often is ordered to look for other conditions like a meniscus tear or ligament damage that may occur with arthritis; and the Blood Tests, although less commonly used, blood tests may be ordered to rule out other diseases. Your doctor may use a small needle to remove a sample of fluid from your knee, which will be sent to the lab for analysis. Results usually are available within 48 hours.
Arthritis is a degenerative disease that destroys the cartilage in a joint. It can be caused by a fracture or other joint injury but also can be hereditary or due to unknown causes. Arthritis most commonly affects the hip, knee, and hand. When arthritis affects a joint, the cartilage loses its smooth, glistening surface and becomes rough and irregular. The result is further destruction of the rest of the joint as the imperfect surfaces contact one another. In response, the joint may attempt to create new bone in the form of bone spurs, which can be quite painful. Eventually, pieces of bone and cartilage can break off and end up floating in the joint fluid, which causes yet further destruction to the once – smooth surfaces. The end result is the partial or complete destruction of the joint.
Osteoarthritis is the most common form of arthritis. Although it can be a hereditary condition, the wear and tear of sports and other activities may increase the risk for osteoarthritis in athletes and active individuals. Osteoarthritis may begin after a specific traumatic injury, as a result of repeated minor injuries or after years of overuse and chronic stress on the knee. Contributing factors that put people at risk of osteoarthritis include:
- Age – The majority of people suffering from arthritis are over 45 years old. By 60, most people have some signs of mild osteoarthritis. However, athletes and active individuals sometimes develop osteoarthritis at a younger age because their active lifestyle places additional stress on their knees.
- Weight – Extra pounds put added stress on your knees. Controlling your weight can help relieve some of the pain associated with arthritis, and also can help you avoid getting arthritis.
- Activities – Both overusing and underusing your knees can increase your risk of osteoarthritis. While overuse can excessively grind down joint cartilage, under use can stiffen and weaken the muscles that help absorb shock.
- Genetics – Some people who suffer from osteoarthritis may have inherited a propensity to develop the disease.
- Abnormal Body Structure – Knees that are not aligned properly or not matched in size, length or strength may cause slight imbalances that increase stress and cause premature arthritis.
- Injury – Trauma can injure the cartilage and prematurely wear out the knee. Ligaments injuries, such as an anterior cruciate ligament (ACL) rupture, also can damage the cartilage.
How To Diagnose Arthritis Knee Pain, Last Update: 16/6/2017